Detecting neuromuscular disorders at an early stage is paramount for managing these conditions effectively and improving the quality of life for those affected. Neuromuscular disorders encompass a wide range of diseases that impair the function of muscles and the nerves that control them. These conditions can lead to significant physical limitations, making timely diagnosis and intervention crucial.
Early detection enables healthcare professionals to implement treatment strategies sooner, which can slow disease progression, alleviate symptoms, and enhance the overall health and mobility of patients. Furthermore, understanding the symptoms and risk factors associated with neuromuscular disorders empowers individuals to seek medical advice promptly, ensuring they receive the necessary care and support. By focusing on early diagnosis, we can make significant strides in mitigating the impact of these challenging and often debilitating conditions.
Understanding Neuromuscular Disorders

Neuromuscular disorders encompass a wide range of conditions affecting the muscles and the nerves controlling them. These disorders interfere with the voluntary muscles’ ability to function and the nerves that communicate sensory information back to the brain. Neuromuscular disorders can be genetic, autoimmune, or acquired through other means, and early detection is essential to managing their impact effectively.
Definition and Types of Neuromuscular Disorders
Neuromuscular disorders occur when there is an issue with the peripheral nerves, the muscles themselves, or the communication between them. Some of the most common types include:
- Muscular Dystrophies: Genetic disorders leading to progressive muscle degeneration and weakness.
- Amyotrophic Lateral Sclerosis (ALS): A disease affecting nerve cells in the brain and spinal cord, resulting in loss of muscle control.
- Multiple Sclerosis (MS): An autoimmune condition impacting the central nervous system, impairing communication between the brain and body.
- Myasthenia Gravis: An autoimmune disorder causing weakness in skeletal muscles.
Common Symptoms and Signs
Identifying neuromuscular disorders can be challenging due to their broad range of symptoms, which often overlap with other conditions. Typical symptoms include:
- Muscle Weakness: Frequently starting in specific muscle groups.
- Muscle Atrophy: Gradual reduction in muscle size and strength.
- Fatigue, Cramps, and Stiffness: Persistent tiredness, involuntary muscle contractions, and joint stiffness.
- Numbness and Tingling: Sensory disturbances indicating potential nerve damage.
Understanding these disorders is the foundation for early diagnosis and intervention, which are critical in mitigating the progression of these conditions and maintaining a better quality of life.
Risk Factors and Causes
Understanding the risk factors and causes of neuromuscular disorders is crucial for early detection and management. These disorders can arise from a variety of genetic, environmental, and lifestyle factors, each influencing the onset and progression of the condition in different ways.
Genetic Factors
Many neuromuscular disorders are inherited, meaning they are passed down from parents to their children through genes. Conditions such as muscular dystrophies, spinal muscular atrophy, and certain types of myopathies are examples where genetic predisposition plays a significant role. In some cases, spontaneous genetic mutations can also lead to these disorders, even in individuals with no family history.
Environmental and Autoimmune Factors
Environmental factors such as exposure to toxins, chemicals, or infections can trigger neuromuscular disorders. For instance, heavy metal poisoning or certain viral infections have been associated with the development of conditions like peripheral neuropathy. Additionally, autoimmune diseases, where the body’s immune system mistakenly attacks its own tissues, can result in neuromuscular disorders such as myasthenia gravis and multiple sclerosis.
Lifestyle and Other Health Conditions
Lifestyle factors, including repetitive motion, poor nutrition, and lack of exercise, can exacerbate the risk of developing neuromuscular disorders. Conditions such as diabetes, hypothyroidism, and other metabolic disorders can also contribute to the onset of these diseases. Maintaining a healthy lifestyle and managing underlying health issues are essential preventive measures.
By identifying and understanding these risk factors, individuals can take proactive steps towards early diagnosis and intervention, potentially reducing the impact of neuromuscular disorders on their lives.
The Role of Early Detection
Early detection of neuromuscular disorders is crucial for optimizing clinical outcomes and enhancing the quality of life for affected individuals. Timely identification and diagnosis of these conditions can significantly alter the disease trajectory, offering better management options and reducing complications.
Benefits of Early Diagnosis
One of the primary benefits of early diagnosis is the ability to initiate treatment sooner. Early intervention, including disease-modifying therapies and symptomatic treatments, can slow the progression of many neuromuscular disorders. This approach not only preserves muscle function longer but also helps in maintaining overall mobility and independence. For instance, in conditions like Duchenne muscular dystrophy (DMD), early detection allows for timely genetic counseling and access to appropriate management strategies, which can substantially improve patient outcomes.
Diagnostic Tools and Techniques
Advancements in diagnostic tools, such as genetic testing and newborn screening programs, have enhanced the ability to detect neuromuscular disorders at an early stage. These technologies help identify genetic mutations linked to specific conditions, facilitating quicker and more accurate diagnoses7. Early detection through these methods ensures that patients receive targeted treatments and appropriate surveillance, thereby minimizing delays in care.
Impact on Long-term Management
Early detection also plays a pivotal role in long-term disease management. It enables healthcare providers to develop personalized care plans tailored to the individual’s specific needs, including physical therapy, nutritional support, and occupational therapy. Furthermore, early diagnosis empowers patients and their families with critical information about the condition, fostering better understanding and proactive health management.
Overall, the role of early detection in neuromuscular disorders cannot be overstated. It is the cornerstone of effective treatment, offering hope and improved quality of life for those affected.
Diagnostic Methods
Accurate diagnosis of neuromuscular disorders is pivotal for early intervention and appropriate management. A variety of diagnostic methods are employed to pinpoint these conditions, ranging from blood tests to advanced imaging and genetic screenings.
Blood Tests and Biochemical Analysis
Initial diagnostic steps often include blood tests to check for elevated levels of muscle enzymes such as creatine kinase (CK). Elevated CK levels can indicate muscle damage, which is common in several neuromuscular disorders. Other biochemical markers may also be assessed to provide further insights into muscle health and metabolic function.
Electrodiagnostic Tests
Electrodiagnostic tests, including electromyography (EMG) and nerve conduction studies (NCS), are critical for evaluating the electrical activity of muscles and the speed of nerve signal transmission. These tests help determine whether symptoms are due to muscle pathology or nerve dysfunction. EMG measures the electrical activity produced by muscles, while NCS evaluates the speed and strength of signals traveling through the nerves.
Imaging Techniques
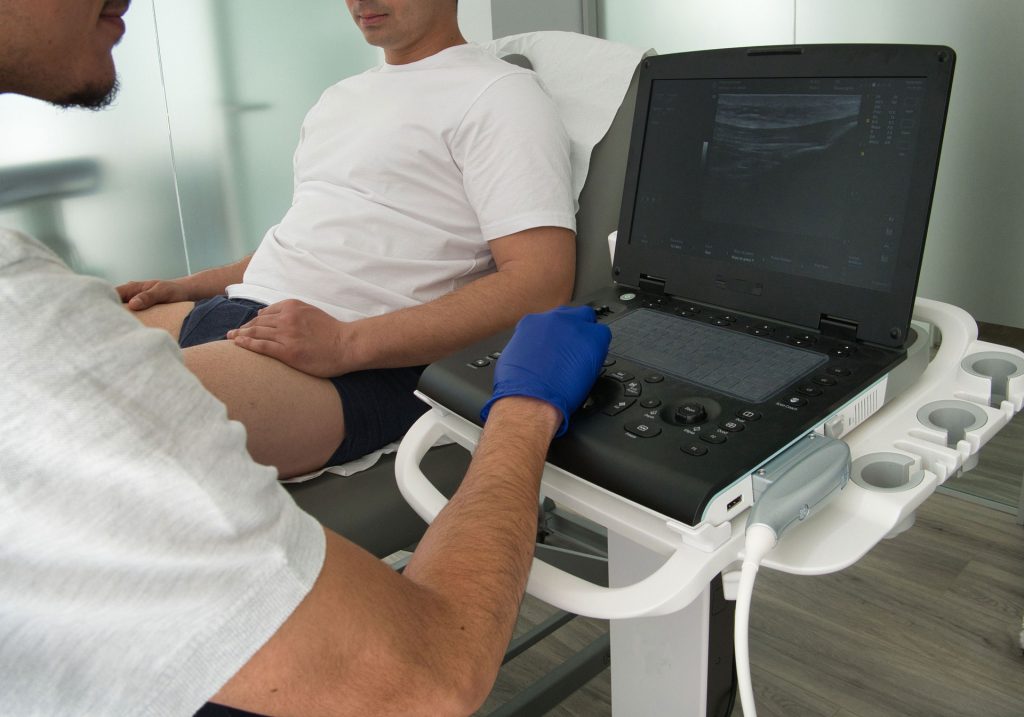
Advanced imaging techniques, such as magnetic resonance imaging (MRI) and computerized tomography (CT) scans, offer detailed views of the brain, spinal cord, and peripheral nerves. These images help detect structural abnormalities that may contribute to neuromuscular symptoms. Neuromuscular ultrasound is another valuable tool, providing real-time images of muscle and nerve structures without radiation exposure.
Genetic Testing
Genetic testing has become a cornerstone in diagnosing inherited neuromuscular disorders. By identifying specific genetic mutations associated with conditions like muscular dystrophies and spinal muscular atrophy, genetic tests facilitate accurate diagnoses and inform treatment plans. Newborn screening programs have also integrated genetic testing to detect these disorders early in life, allowing for prompt intervention.
Lumbar Puncture
In some cases, a lumbar puncture (spinal tap) may be performed to analyze cerebrospinal fluid. This test can reveal abnormalities in the central nervous system, such as inflammation or infections, which might contribute to neuromuscular symptoms.
Comprehensive diagnostic methods are essential for accurately identifying neuromuscular disorders. Early and precise diagnosis enables tailored treatment strategies, improving patient outcomes and quality of life.
Treatment Options
While there is currently no cure for neuromuscular disorders, various treatment options can help manage symptoms, slow disease progression, and improve the quality of life. Early detection plays a critical role in optimizing these treatments and enhancing patient outcomes.
Medical Therapy
- Medications: Various medications are used to manage neuromuscular disorders. For example, Riluzole is commonly prescribed for Amyotrophic Lateral Sclerosis (ALS) to slow the disease’s progression. Immunosuppressive drugs, such as corticosteroids, are used to reduce inflammation in conditions like myasthenia gravis.
- Pain Management: Pain management strategies may include steroid injections to alleviate nerve-related pain in the back and neck. Other analgesics and antispasmodics are also used to control pain and muscle spasms.
Physical and Occupational Therapy
- Physical Therapy: Physical therapy is essential for restoring muscle tone, maintaining mobility, and preventing contractures. Therapeutic exercises tailored to the patient’s condition can enhance muscle strength and function.
- Occupational Therapy: Occupational therapy focuses on improving daily living skills and adapting environments to ensure patient safety and independence.
Advanced Therapeutic Procedures
- Apheresis: Apheresis, or plasmapheresis, is a procedure that filters the blood to remove harmful antibodies, often used in autoimmune neuromuscular disorders.
- Genetic Therapies: Research is ongoing into genetic therapies aimed at correcting the underlying genetic defects responsible for certain neuromuscular disorders.
Assistive Devices
- Mobility Aids: Using assistive devices such as braces, wheelchairs, and walkers can significantly improve mobility and independence for individuals with severe muscle weakness.
- Communication Aids: For patients with speech difficulties, communication devices and alternative communication methods can facilitate better interaction with others.
Comprehensive Care
Neuromuscular disorder treatment often requires a multidisciplinary approach involving neurologists, physical therapists, occupational therapists, and pain specialists. Early detection allows for the timely initiation of these treatments, improving long-term outcomes and quality of life for patients.
When to Seek Specialist Consultation
Recognizing when to seek specialist consultation for neuromuscular disorders is critical for early diagnosis and effective management. Early intervention can significantly improve outcomes, so understanding the signs that warrant professional evaluation is vital.
Key Signs to Watch For
Individuals experiencing any of the following symptoms should consider seeking a specialist consultation:
- Persistent Muscle Weakness: Unexplained or progressive muscle weakness in the arms or legs can be an early indicator of a neuromuscular disorder.
- Muscle Cramps and Twitching: Frequent cramps or muscle twitching not related to physical activity could point to underlying nerve issues.
- Numbness and Tingling: Chronic numbness or tingling sensations in the extremities may suggest nerve damage and should be evaluated promptly.
- Difficulty with Motor Skills: Problems with coordination, balance, or performing everyday tasks such as walking or gripping objects.
Benefits of Early Specialist Consultation
Seeking a specialist consultation early can lead to:
- Accurate Diagnosis: Specialists employ advanced diagnostic methods to accurately identify the specific neuromuscular disorder.
- Tailored Treatment Plans: Early diagnosis allows for personalized treatment strategies, including medication, physical therapy, and lifestyle modifications.
- Improved Prognosis: Timely intervention can slow disease progression and enhance the quality of life.
If you are experiencing any of these symptoms, it is essential to consult a specialized neuromuscular center. The Maryland Neuromuscular Center in Columbia, Maryland, offers comprehensive care and cutting-edge diagnostic tools for managing neuromuscular disorders. Experts at the center provide tailored treatment plans designed to address each patient’s unique needs.
